Impetigo Treatment in
Marietta & East Cobb
Board-certified dermatology care for impetigo in children and adults – fast-acting antibiotic therapy, infection control, and strategies to prevent spread and recurrence.
What Is Impetigo?
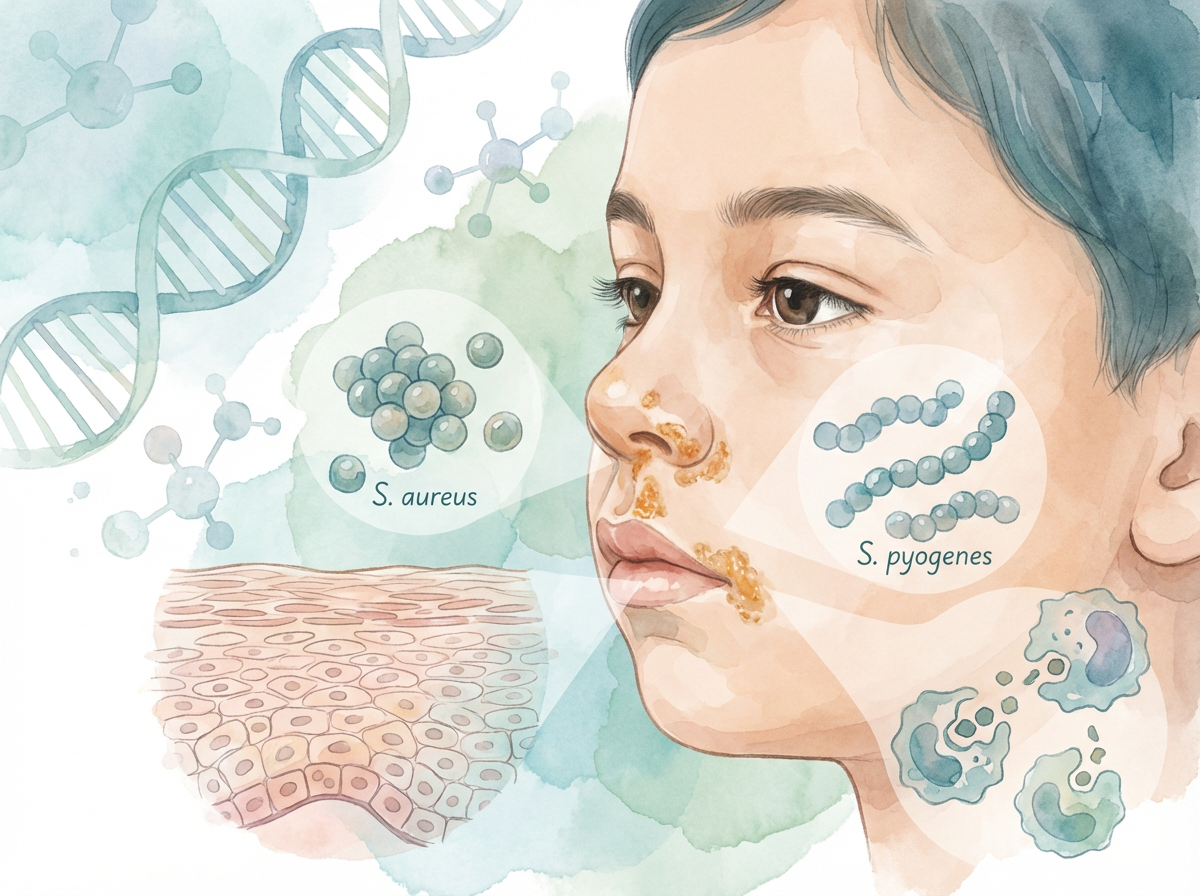
Impetigo is a common, highly contagious bacterial skin infection that primarily affects infants and young children, though it can occur at any age. It is caused by Staphylococcus aureus or Streptococcus pyogenes bacteria that enter the skin through small breaks, cuts, or insect bites.
The infection produces characteristic honey-colored crusted sores that spread easily through direct contact, shared towels, or contaminated surfaces. Without treatment, impetigo can spread to other parts of the body and to other people – making prompt diagnosis and treatment essential.
At DESSNA, we provide rapid diagnosis and effective antibiotic therapy for all forms of impetigo, along with guidance to prevent spread within families, schools, and daycare settings.
Types of impetigo we treat
Non-Bullous Impetigo
The most common form, accounting for about 70% of cases. Begins as small red sores around the nose and mouth that quickly rupture, ooze, and form characteristic honey-colored crusts. Highly contagious through direct contact.
Bullous Impetigo
Caused specifically by Staphylococcus aureus toxins. Produces larger, fluid-filled blisters (bullae) on the trunk, arms, and legs that rupture and leave thin, varnish-like crusts. More common in infants and young children.
Ecthyma
A deeper, more serious form of impetigo that penetrates into the dermis. Creates painful, pus-filled sores with thick crusts that can leave scars. Requires more aggressive treatment than superficial forms.
Secondary Impetigo
Bacterial infection that develops on skin already compromised by another condition – such as eczema, insect bites, cuts, or chickenpox. The pre-existing break in the skin barrier allows bacteria to colonize and spread.
Why Impetigo Develops
Impetigo occurs when bacteria exploit a break in the skin's protective barrier. Understanding how it spreads is essential for effective treatment and prevention.
Bacterial Infection
Impetigo is caused by Staphylococcus aureus (most common) or Streptococcus pyogenes bacteria. These organisms colonize the skin surface and invade through any break in the skin barrier – even microscopic ones.
Breaks in the Skin Barrier
Cuts, scrapes, insect bites, eczema patches, chickenpox lesions, and even minor skin irritation create entry points for bacteria. Children with active eczema are particularly susceptible to secondary impetigo.
Close Contact & Crowding
Impetigo spreads easily in schools, daycare centers, sports teams, and households through direct skin-to-skin contact, shared towels, clothing, and contaminated surfaces. Warm, humid conditions accelerate spread.
Compromised Immunity
Children, elderly individuals, and those with weakened immune systems or chronic skin conditions are more vulnerable. Poor hygiene, malnutrition, and crowded living conditions also increase risk.
How We Treat Impetigo at Our Marietta Practice
We resolve the active infection quickly, prevent spread to others, and address any underlying conditions that made the skin vulnerable in the first place.
Clinical Diagnosis
Your dermatologist examines the sores to confirm impetigo and determine the type (non-bullous, bullous, or ecthyma). We assess the extent of infection, check for signs of deeper involvement, and evaluate whether culture and sensitivity testing is needed – particularly if the infection hasn't responded to initial treatment.
Targeted Antibiotic Therapy
Based on the type and severity, we prescribe the most effective antibiotic approach. Localized cases respond well to topical antibiotics (mupirocin or retapamulin), while widespread or resistant infections require oral antibiotics. Culture-guided therapy ensures we target the specific bacteria causing your infection.
Spread Prevention & Follow-Up
We provide detailed guidance on preventing transmission to family members, classmates, and teammates – including hygiene protocols, return-to-school timelines, and wound care instructions. Follow-up ensures complete resolution and addresses any underlying skin conditions that may have predisposed to infection.
Impetigo Treatment Options at Our Marietta Practice
Your treatment is tailored to the type, extent, and severity of infection, with a focus on rapid resolution and preventing spread to others.
Topical Antibiotics
Mupirocin (Bactroban) or retapamulin ointment applied directly to affected areas after gentle crust removal. Topical antibiotics are first-line treatment for limited impetigo with fewer than 5 lesions and no systemic symptoms.
Oral Antibiotics
Oral antibiotics (cephalexin, dicloxacillin, or amoxicillin-clavulanate) for impetigo that is widespread, bullous, ecthyma, or not responding to topical treatment. Course typically lasts 7 – 10 days.
MRSA-Targeted Therapy
Culture-guided antibiotic selection for methicillin-resistant Staphylococcus aureus. Options include trimethoprim-sulfamethoxazole, clindamycin, or doxycycline based on local resistance patterns and culture results.
Wound Care & Crust Removal
Gentle soaking and removal of honey-colored crusts to improve antibiotic penetration and accelerate healing. We provide detailed wound care instructions including proper cleansing technique and bandaging.
Underlying Condition Treatment
When impetigo develops on skin compromised by eczema, insect bites, or other conditions, we treat both the infection and the underlying condition to prevent recurrence and restore the skin barrier.
Decolonization Protocol
For patients with repeated episodes, a structured decolonization regimen targeting nasal and skin Staph carriage – including mupirocin nasal ointment and chlorhexidine washes – can break the cycle of reinfection.
Preventing Impetigo from Spreading
Impetigo is highly contagious. These steps are essential to prevent transmission to family members, classmates, and teammates:
Wash hands frequently with soap
Keep lesions bandaged and clean
Towels, razors, clothing, bedding
Prevent scratching and spreading
Until 24 hours after starting antibiotics
Why Professional Diagnosis Matters
Impetigo vs. Cold Sores
Cold sores (herpes labialis) and impetigo can both appear around the mouth and nose. However, cold sores are caused by HSV-1 virus and require antiviral treatment, while impetigo is bacterial and requires antibiotics. Using the wrong treatment delays healing and allows the infection to spread.
Impetigo vs. Eczema
Eczema and impetigo can coexist – and eczema-affected skin is particularly vulnerable to bacterial infection. Distinguishing between an eczema flare and secondary impetigo is critical because treatment differs significantly. Steroids alone can worsen an active bacterial infection.
If your child has sores that are spreading, crusting, or not healing with home care, a dermatologist evaluation ensures the right diagnosis and the right treatment – preventing complications and protecting others.
What Our Patients Say
“Doctor Edward Chen is the BEST! He's very professional, very caring, he will always give you his honest advice. He helped my son who had acne issues – his skin now looks great like never before.”
“Dr. Candace Green has a very warm bedside manner and makes you feel very comfortable! Great office, staff, and overall experience.”
“The office is well run and Dr. Green is thorough.”
Impetigo Treatment FAQs
Answers to the questions our Marietta and East Cobb patients ask most about impetigo care.
Yes, highly. Impetigo spreads through direct skin-to-skin contact with an infected person's sores, or through shared items like towels, clothing, and bedding. It can also spread to other parts of your own body by touching or scratching the sores. Children are contagious until 24 hours after starting antibiotic treatment or until sores have completely crusted and healed.
Concerned About Impetigo in Marietta or East Cobb?
Don't let the infection spread. Our board-certified dermatologists provide fast, effective treatment for impetigo in children and adults – with clear guidance on preventing transmission to family members and classmates.
Most patients see significant improvement within 2 – 3 days of starting treatment.
Related Conditions & Services
Explore other infectious and inflammatory skin conditions we treat at our Marietta practice
